Common problems
It is normal to experience some discomforts in pregnancy. The minor discomforts are often short-lived and your midwife or doctor will advise and reassure you about how to deal with them. Sometimes they can become quite severe if this occurs you may need to talk to your doctor about what to do. Some of most common discomforts/concerns are:
Backache
This can occur at any stage during pregnancy due to hormonal changes that loosen your ligaments and as your baby grows your posture is affected. There is also extra strain on your joints and hips as you generally gain weight as you get closer to the birth. Gentle exercise, maintain good posture and taking care while lifting can help prevent back pain.
Helpful tips:
- wear flats shoes
- sit and stand tall with your shoulders relaxed
- bend at the knees when lifting & avoid heavy lifting
If you are experiencing backache or pain around your pelvis, see our factsheet: Pelvic and lower back pain in pregnancy and after birth.
Bladder Problems
Many women experience the need to empty their bladder frequently during pregnancy. This desire to pass urine may be caused by hormonal changes in early pregnancy. In late pregnancy, this is generally caused by the weight of your growing baby pressing on your bladder.
If you notice any discomfort, burning or foul smelling urine with frequent passing of urine, it is important to talk to your doctor or midwife as you may have an infection requiring treatment.
Some women begin to experience leakage of urine during pregnancy when they cough, sneeze, laugh, lift or exercise. This is called stress urinary incontinence. This is common but not normal. It often occurs due to having weak pelvic floor muscles. It is important to strengthen these muscles. To learn more about the pelvic floor and prevention of bladder problems please visit the Continence Foundation of Australia or refer to pelvic floor muscles in pregnancy.
Tips for a healthy bladder:
- Drink 6-8 cups (1.5-2 litres) of fluid a day unless otherwise advised by your doctor
- Spread your drinks evenly throughout the day
- Drink more fluids (preferably water) if the weather is hot or if you are exercising
- Cut down on sugary drinks and drinks that have caffeine in them as they can irritate the bladder
- Don’t reduce your fluid intake if you have a bladder control problem as this will concentrate your urine and could make your problem worse
- Go to the toilet when your bladder feels full. Don’t get into the habit of going “just in case”
- Sit down on the toilet and relax, don’t squat or hover.
To learn more about the bladder, pelvic floor, pregnancy or post birth related topics please visit The Pregnancy Guide,
If you would like help with a bladder problem, speak with your doctor or midwife about a referral to a physiotherapist.
Bleeding gums
This is called ‘pregnancy gingivitis’. Pregnancy hormones effect the gums and even a small build-up of plaque can cause irritation and bleeding. You can help prevent gingivitis by brushing your teeth twice daily with fluoride toothpaste and flossing regularly. You are also encouraged to visit your dentist in pregnancy.
Constipation
The muscles in the bowel can slow down because of pregnancy hormones which for some women may cause constipation. You can tackle constipation by:
- eating a fibre rich diet e.g. vegetables, fruit, and wholegrain bread
- drinking plenty of fluid
- taking a fibre supplement if required
- exercising regularly e.g. swimming or walking
Please be aware that some iron tablets can cause constipation and that laxatives are not advised. If you are suffering with constipation you may need to speak to a doctor about a different brand of iron tablet or use of laxatives.
Practise good toilet habits.
- Wait for the urge to open your bowels.
- Get into the correct sitting position on the toilet – this helps to fully relax your pelvic floor and sphincter muscles.
- sit on the toilet
- elbows on knees
- lean forward
- support feet with a footstool
To learn more about good toilet habits click here.
If things don’t improve – talk to your GP or midwife.
Cramps
Muscle cramps are very common during pregnancy, especially at night. They most commonly occur in the calf muscle but can also happen in the foot or thigh.
You can try to relieve the cramp using massage and stretching. Hold each stretch for 2 minutes. See pictures below of how to stretch your calf muscle. It is helpful to do these stretches before bed each night in order to prevent cramping.
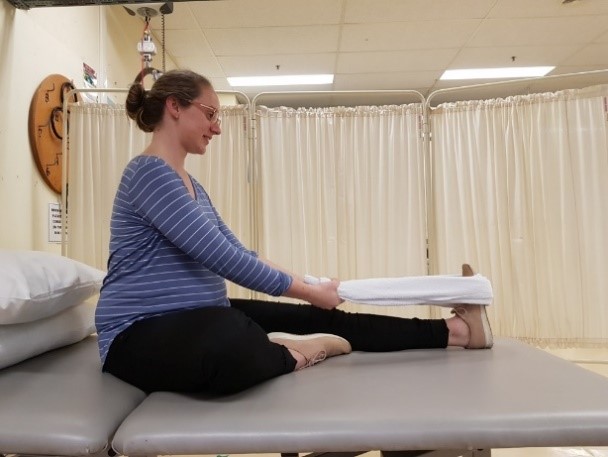

Heartburn
Heartburn, also known as indigestion is common during pregnancy and thought to be triggered by hormonal changes as well as the growing baby pressing on your stomach. It is a burning sensation in your chest and throat, and can also cause a bitter taste or reflux in the mouth. Avoiding strong tea or coffee, pure fruit juice, fried, spicy and fatty foods, drinking during meals, and eating slower can lessen the symptoms. If you experience heartburn during the night try sleeping more upright and well supported with pillows.
Morning sickness
The feeling of nausea and sickness usually starts about the sixth week of pregnancy and settles around the fourteenth week, can occur at any time of day and sometimes can continue on during pregnancy. You will hear this referred to as ‘Morning Sickness’. Again this feeling is linked to pregnancy hormones but the cause is unknown. These tips may help:
- If you tend to feel really sick in the morning, eat a little as soon as you wake up and before getting out of bed and take your time getting out of bed. Ask someone in your household to bring some food to you, or place a snack beside your bed.
- Drink plenty of fluids, preferably 10 to 12 glasses – frequent small amounts are generally tolerated better than larger amounts at once. Fluids such as sports drinks, diluted fruit juice or cordial are usually more effective than plain water. Suck on icy poles or ice if other fluids cannot be tolerated.
- Ginger can often help to relieve nausea. Try dry ginger ale (non-alcoholic) sliced fresh ginger in hot drinks or ginger tablets generally available over the counter..
- Try to eat small meals more frequently rather than large meals
- Try to avoid an empty stomach by snacking on dry biscuits, fruit, barley sugar or have salty snacks available for when nausea occurs.
- Avoid rich, fatty or spicy foods, chocolate and caffeine
- The smell of hot food may lead to feeling sick –try eating cold food.
- Limit the time preparing food as you may not actually feel like eating it by the time it is ready
- Make sure you get enough rest- several times per day if able, and have some fresh air and sunlight each day
If you experience ongoing and excessive vomiting, called ‘hyperemesis gravidarum’ or are losing weight, it is important that you visit a doctor to check that you are not becoming dehydrated. There are a number of medications that doctors can prescribe that when taken regularly can help relieve the symptoms. In severe cases where you may be unable to take in enough fluid, a short stay in hospital is sometimes required for rehydration with an intravenous drip.
Some women may choose alternative and complementary options and approaches to help with morning sickness. Whilst there is very good evidence to support the effectiveness of some of these treatments, there are also some alternative treatments where the evidence varies. Some of these treatments will either be just ineffectual and expensive but be aware that some can actually be harmful to your pregnancy or affect medicines you are taking. You can discuss any of these treatments with your midwife or doctor.
Pelvic girdle pain
Pelvic, lower back, hip, thigh and groin pain are very common during pregnancy. Women may experience an ache, locking, clicking or grinding sensation. Particularly when rolling in bed, walking or standing on one leg. This can happen due to the changes in body shape, posture, increased pressure on the pelvis and hormones increasing the flexibility of the joints in preparation for child birth.
Pregnancy related pelvic / lower back pain often resolves naturally soon after having your baby. For some useful strategies to help manage this pain see the fact sheet: Pelvic and lower back pain during pregnancy and after birth.
If you need further advice, talk to your midwife for a referral to a physiotherapist.
Skin changes and itching
The skin of your tummy gets tighter and can start to feel slightly itchy as your baby grows. Contact your doctor or midwife if itching persists or becomes more severe as this can be a sign of a more serious problem.
Pregnancy hormones cause skin changes due to extra blood circulating around your body. The tone and colour can change, and for some women their skin will 'glow'. Some women may develop red patches, acne may get worse and areas of skin may become dry and scaly. You may notice more pigmentation across areas of your face called Chloasma, otherwise called the ‘mask of pregnancy’.
Moles, freckles and the areola (nipples) of the breasts can be affected by increased pigmentation, and the skin of genitalia, inner thighs, under eyes and armpits may also become darker. A dark line along the midline of the tummy may develop in some women called the linea nigra. After birth, the deeper pigmented skin will remain darker for some time but will gradually fade and disappear.
The majority of women get stretch marks, usually across the abdomen but can also affect thighs, hips, breasts and upper arms. Stretch marks initially appear as prominent red streaks during pregnancy, but gradually fade to pale silvery streaks in the months following birth.
Swelling of hands and feet
The majority of pregnant women will experience some swelling in their ankles, feet and fingers particularly at the end of the pregnancy. This is caused by the extra fluid in your body during pregnancy which may collect in your legs particularly you stand for long periods of time and especially during hot weather. It typically increases throughout the day and usually reduces overnight. If you notice increased swelling of your legs and feet, try reducing prolonged standing, wear comfortable loose shoes and put your feet up when resting.
Sometimes fluid collecting in the wrists produces painful or tingling sensations in the fingers. This is called ‘carpal tunnel syndrome’. Speak to your midwife or doctor if this concerns you.
Swelling (oedema) can sometimes be a sign of high blood pressure and pre-eclampsia. Tell your midwife or doctor if the swelling is not relieved by resting with feet up, occurs elsewhere in your body or becomes excessive.
Tiredness and difficulty sleeping
Frequent need to go to the toilet, suffering from heartburn, your baby moving around or just a general feeling of discomfort when you lie down can all disturb sleep during pregnancy. Approaching childbirth and parenthood can produce some anxiety causing some women to experience unsettling dreams or even nightmares especially later in pregnancy.
If you are having trouble sleeping or tiredness, you may like to try:
- Resting during the day: lie on your side with a pillow under your tummy and another between your knees.
- Avoiding tea and coffee before bedtime.
- Exercising during the day.
- Relaxing before bed by soaking in a bath, listening to music, having a massage or meditating.
Vaginal thrush
Nearly all women will experience an increase in vaginal discharge during pregnancy. Any discharge that has an unpleasant odour, causes soreness, itching or is discoloured, may indicate a vaginal thrush infection and it is important to see your doctor for treatment.
Varicose veins and Hemorrhoids
These are swollen veins, usually in the legs, but sometimes in the vulva (vaginal opening) or rectum and anus. They may cause aching and sometimes itching. Support tights can help varicose veins in the legs, and try to avoid standing for long periods. Rest with your legs up when you can. Always tell your midwife or GP if you notice any hot, red or painful areas in your legs or vulva.
Hemorrhoids are varicose veins of the rectum or anus. They can feel sore and may become swollen. It can become difficult and uncomfortable to go to the toilet and they may become worse with constipation. Your midwife or GP can advise on dietary changes and available treatments.
Last Modified: Monday, 29 March 2021
